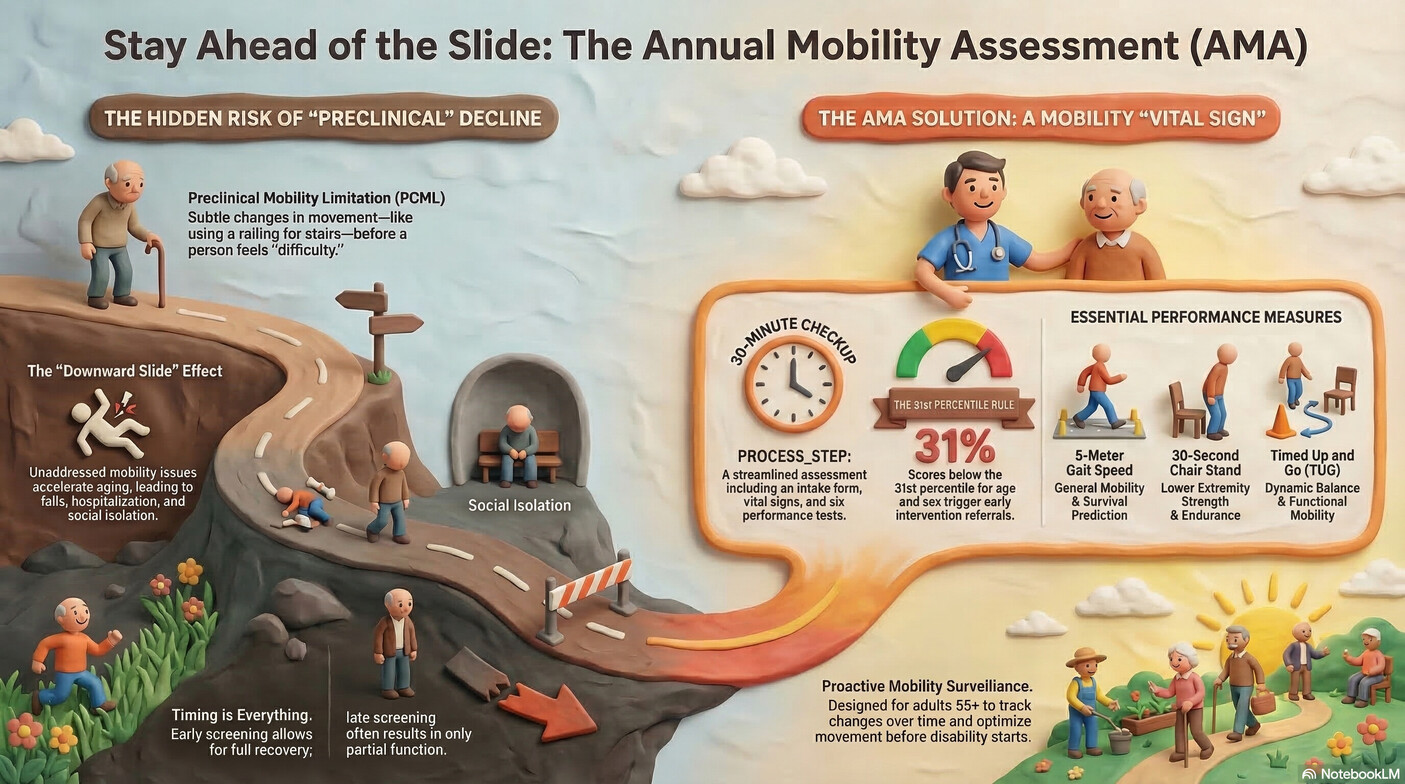
We often view aging as a slow, inevitable decline, yet we rarely intervene until a crisis—like a fall or a hospital stay—forces our hand. In reality, there is a "downward slide" toward frailty and loss of independence that begins much earlier than most realize. This trajectory is fueled by a "funnel" of compounding factors: acute injuries, poorly managed chronic conditions, and inactivity.
To combat this, the American Physical Therapy Association (APTA) Academy of Geriatric Physical Therapy has proposed the Annual Mobility Assessment (AMA). Think of it as a movement surveillance system designed to catch subtle shifts in your physical health long before they become permanent disabilities. This shift from reactive rehabilitation to proactive longevity strategy is essential for anyone serious about maintaining their quality of life.
Takeaway 1: The "Preclinical" Warning Sign You’re Likely Ignoring
The most dangerous stage of decline is the one you cannot feel. Clinicians call this Preclinical Mobility Limitation (PCML), a phase where you can still perform a task, but your method of doing so has secretly changed. You might start using a railing on the stairs or walking more slowly, yet you don't perceive any "difficulty" or "limitation" yet.
Identifying this decline at "Point A" on the functional curve is critical because it occurs while you still possess significant physiologic reserve. If you wait until "Point B"—where you finally admit you have trouble moving—the cost of recovery is higher and the likelihood of a full return to function is lower. By recognizing these altered movement patterns early, physical therapists can intervene before the slide toward disability becomes inevitable.
"Preclinical mobility limitation is defined as experiencing some change in the ability to perform mobility, but not yet perceiving any level of difficulty."
Takeaway 2: Your Movement Needs a "Vital Sign"
Currently, the primary tool for senior health is the Medicare Annual Wellness Visit, which is often limited to a 20-minute review of medications and subjective self-reporting. Research shows this "just asking" approach is inadequate, failing to catch early physical loss that patients haven't yet noticed. Your movement requires objective data, similar to how we monitor blood pressure or cholesterol.
The AMA establishes a "mobility vital sign" through six performance-based measures. These aren't just simple walking tests; they are designed to assess the "roots" of your mobility, including lower extremity strength, power, endurance, and even the "divided attention" required for cognitive dual-tasking. These objective benchmarks include:
- Self-selected and Fast gait speeds
- 30-second chair stand test
- Timed Up and Go (TUG)
- TUG with a cognitive dual task
- Four-Square Step Test
Takeaway 3: The "Dental Model" of Physical Therapy
The task force behind the AMA argues that our physical health should follow the "dental model" of primary prevention. We don't wait for a tooth to fall out before seeing a dentist; we go for routine cleanings to prevent "movement cavities" from forming in the first place. This approach shifts the physical therapist’s role from a rehabilitation specialist to a "longevity coach" who optimizes your movement patterns.
By establishing a baseline while you are still healthy, your therapist can provide specific physical activity counseling to prevent future decline. This proactive surveillance aims to transform society by optimizing movement before a crisis occurs. It is an investment in your future self, ensuring that your body remains a capable vessel for your lifestyle for decades to come.
Takeaway 4: Why "Average" Performance Can Be Deceptive
Relying on "pass/fail" fall-risk thresholds can be a dangerous mistake for active adults. For instance, a 55-year-old man walking at 1.02 meters per second is technically "safe" on a standard test, but he is actually performing significantly below the average for his age and sex (1.31 m/s). That same speed is considered normal for an 85-year-old, meaning the 55-year-old is already losing vital physiologic reserve.
The AMA framework uses age- and sex-specific percentiles to identify the "amber light" of decline. Performing below the 31st percentile (0.5 standard deviations below the mean) indicates that you are likely in the PCML stage, even if you feel fine. This specific, data-driven approach catches people in the "PCML likely" category before they hit the high-risk "red zone" of actual mobility limitation.
Takeaway 5: You Probably Want This Data More Than Your Doctor Realizes
There is a staggering gap between what the medical system provides and what health-conscious adults actually value. While primary care physicians document mobility limitations in only 2% of visits, 100% of participants in mobility checkup studies found the assessments "useful" and were willing to pay out of pocket for them. Patients prioritize their independence and want to know their "mobility status" long before they reach age 60.
Contrast this high demand with the fact that only 23% to 25% of seniors utilize the current Medicare Annual Wellness Visit. The traditional medical model is failing to meet the public’s desire for proactive, functional health data. People aren't just looking for an absence of disease; they are looking for the data-driven assurance that they can continue to move, engage, and live well.
"Physical therapists should not wait until a perfect model is unveiled to address this epidemic."
Conclusion: The Future of Optimal Aging
The Annual Mobility Assessment represents a necessary evolution in how we manage the aging process. By treating mobility as a vital sign, we can transition from a society that manages disability to one that cultivates longevity. This shift is already gaining legislative momentum through the Stopping Addiction and Falls for the Elderly (SAFE) Act, which seeks to expand access to essential fall screenings and prevention.
Optimizing your movement trajectory is the single most important thing you can do for your future independence. As we move toward a healthcare model that values prevention as much as the cure, it’s time to look beyond the scale and the blood pressure cuff. Do you know your "mobility numbers," and do you know which way your trajectory is trending?