The modern wellness marketplace is currently inundated with red light devices, ranging from LED face masks promising eternal youth to "healing belts" promoted by social media influencers.
For the clinician-scientist, this saturation of high-gloss marketing and hyperbolic claims often triggers a necessary skepticism. However, beneath the layer of consumer "biohacking" lies a robust biological foundation that is rapidly shifting from the medical periphery into the core of evidence-based neurorehabilitation.
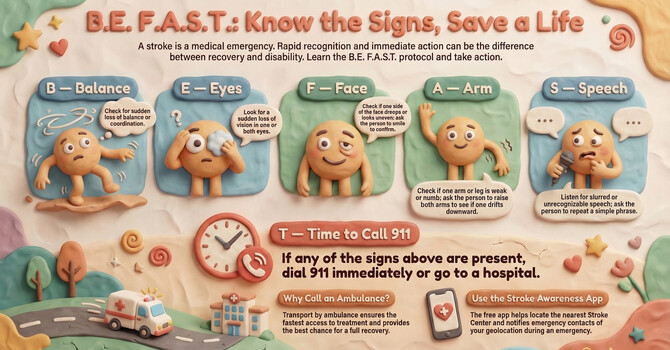
This transition from "fringe" to "mainstream" is perhaps best exemplified by the clinical journey of Dr. David Ozog. In 2021, when his son suffered a massive stroke that resulted in partial paralysis, Ozog—a dermatologist—moved past his initial professional doubt. Influenced by research from the Department of Defense, he began "sneaking" LED panels into the hospital to provide near-infrared light to his son’s head, hoping to achieve some level of neuroprotection.
Today, while his son’s recovery cannot be attributed to a single variable, the experience highlights a pivotal shift in clinical perception. What was once dismissed as "shining a flashlight on a wound" is now understood as a precise method of influencing cellular metabolic demand. As neuro-rehabilitators, we are moving away from anecdotal observation toward a rigorous understanding of how light interacts with human physiology at a molecular level.
Defining the Mechanism: What is Photobiomodulation?
In a clinical context, "red light therapy" is more accurately termed Photobiomodulation (PBM). This process involves the application of specific wavelengths of light, primarily within the "optical window" of 600 nanometers (nm) to 1,100 nm. Unlike surgical lasers that rely on thermal energy to cut or ablate tissue, PBM is strictly non-thermal.
The efficacy of PBM relies on the fact that longer wavelengths, such as red and near-infrared light, scatter significantly less than shorter wavelengths like blue or ultraviolet light. This allows photons to penetrate centimeters into the tissue, reaching muscles, nerves, and even deep-seated neural structures. It is a biological intervention that uses light as a fuel source rather than a heat source.
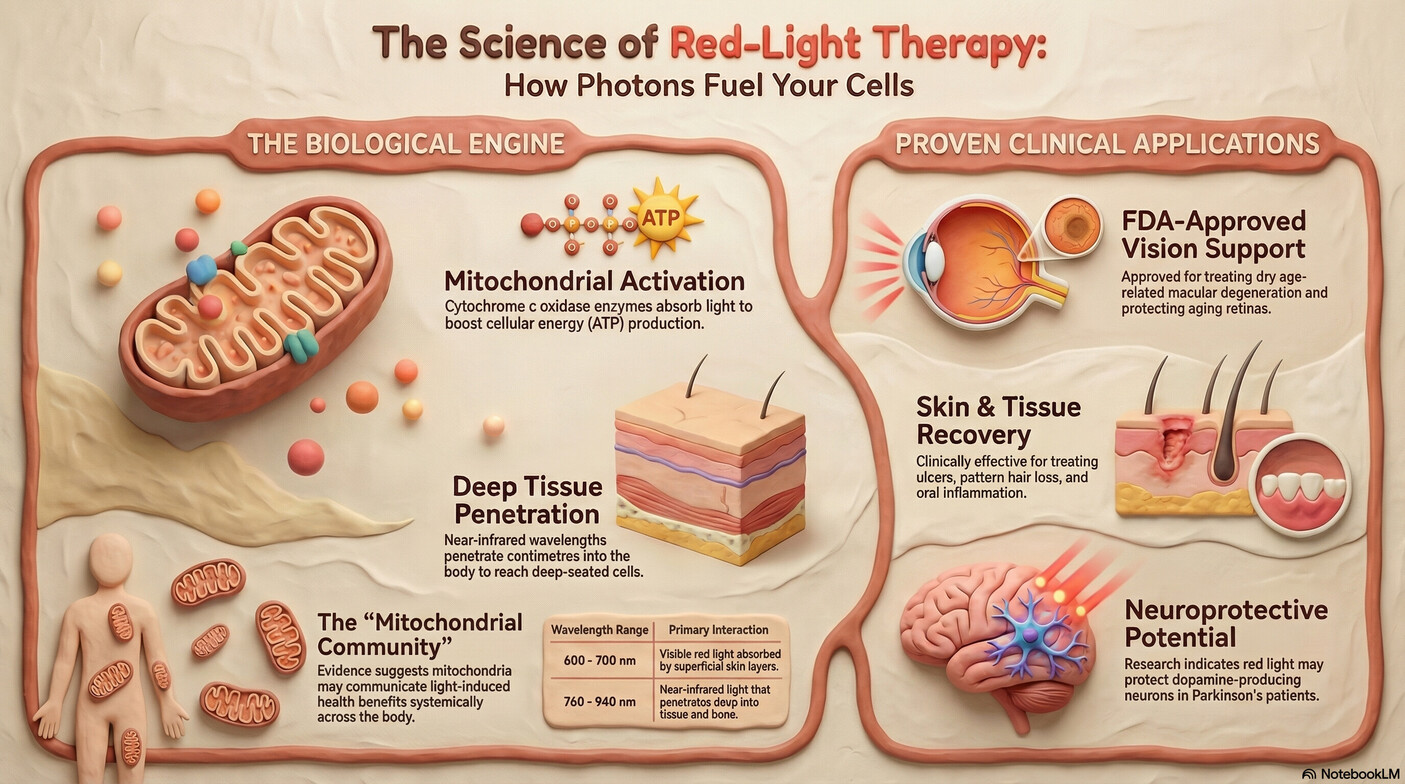
By utilizing these specific ranges—often targeting the 600–700 nm and 760–940 nm bands—we can trigger localized and systemic chemical changes. For the neuro-rehabilitator, this provides a non-invasive tool to support tissue that is metabolically stressed or neurologically compromised.
The Biological Engine: Mitochondrial Optics and ATP Production
To understand why PBM works, we must analyze the "cellular power plants," the mitochondria. These organelles are responsible for producing adenosine triphosphate (ATP), the chemical energy currency required for every metabolic process, including neuroplasticity and motor learning. Within the mitochondrial electron transport chain resides an enzyme called cytochrome c oxidase, which serves as a primary light receptor.
When photons from the red and near-infrared spectrum are absorbed by cytochrome c oxidase, they nudge the mitochondrial machinery into a higher state of activity. This interaction effectively "recharges" the cellular battery by accelerating the flow of electrons and increasing the metabolic throughput of ATP. This is not merely a boost in energy; it is an optimization of the cell’s ability to perform its specialized functions.
Recent research suggests a sophisticated "lubricant" analogy for this process. It appears that red light reduces the viscosity of the water surrounding the mitochondrial engine. This reduction in resistance allows the ATP synthase—essentially a biological molecular turbine—to rotate more easily and efficiently. By lowering the physical friction within the cell's energy-producing machinery, we can facilitate faster recovery and more robust cellular signaling.
What the Research Demonstrates: A Clinical Evidence Review
The scientific literature for PBM has matured significantly, moving beyond simple wound healing into complex systemic interventions. A major 2025 consensus review involving over 20 specialists confirmed that PBM is both safe and effective for conditions like peripheral neuropathy, acute radiation dermatitis, and androgenic alopecia. Furthermore, the FDA has recently approved red light devices for treating dry age-related macular degeneration, marking a milestone for optical therapy.
The implications for systemic health are equally striking. A 2022 study in Brazil demonstrated that patients with severe COVID-19 who received daily PBM left the hospital an average of four days earlier than the control group. Additionally, research by neuroscientist Glen Jeffery has shown that just 15 minutes of red light exposure on a patient’s back can blunt post-meal blood sugar spikes, suggesting a "distal effect" where mitochondria communicate across the body.
In the realm of neurorehabilitation, the pursuit of "neuroprotection" remains the holy grail. Animal models of Parkinson’s disease have shown that PBM can preserve dopamine-producing neurons, a finding that has led to human trials using transcranial devices and optical fibers. These studies suggest that PBM may alter "biophotons"—faint light signals produced by cells—to signal health and resilience across neural networks, potentially making an older or injured brain function more like a younger, healthy one.
The Science of Dosing: Navigating the Arndt-Schulz Curve
A common critique of PBM is the variability in clinical results, which usually stems from a misunderstanding of the "Biphasic Dose Response," often referred to as the Arndt-Schulz Curve. In photobiomodulation, more is not necessarily better. There is a biological "sweet spot" where the dose is sufficient to trigger a therapeutic response; however, exceeding this threshold can lead to an inhibitory effect, effectively "turning off" the benefits.
This is why at-home consumer devices frequently fail to produce clinical-grade results. Most consumer masks and belts lack the power density (irradiance) required to penetrate through the human skull or deep into large muscle groups. Precision in wavelength, intensity, and duration is non-negotiable for achieving a meaningful therapeutic outcome, especially when attempting to influence deep-seated neurological tissues.
Clinicians must also account for variables such as skin pigment and tissue density, which influence how photons are absorbed or reflected. In a professional setting, we calculate the exact "joules" of energy delivered to ensure we remain within the therapeutic window. Without this precision, the therapy is little more than expensive ambient lighting.
Integration at Unity Move Physical Therapy & Wellness
At Unity Move Physical Therapy & Wellness, we do not view PBM as a passive, standalone "treatment." Instead, we utilize it as a "metabolic primer." By applying targeted red and near-infrared light to compromised tissues before a session, we optimize the cellular environment for the rigors of physical rehabilitation.
Our philosophy centers on the fact that humans in the modern era are "light starved." We spend the majority of our time indoors under energy-efficient lighting that has been stripped of the restorative red and near-infrared wavelengths we evolved to receive. By restoring this spectrum, we can reduce oxidative stress and systemic inflammation, creating a foundation for more effective motor learning and neuroplasticity.
We integrate PBM with individualized movement-based therapy to maximize the patient's recovery potential. When the cellular "engine" is properly lubricated and fueled with ATP, the physical work of rehabilitation—whether it is gait training after a stroke or strength recovery after surgery—becomes more efficient. We are not just treating symptoms; we are enhancing the biological capacity for movement.
Who Stands to Benefit?
Based on current clinical data and our own internal protocols, several patient profiles are ideal candidates for integrated PBM:
- Chronic Pain and Musculoskeletal Management: Patients with osteoarthritis, fibromyalgia, or chronic low back pain often see a modulation in inflammatory markers and significant pain relief.
- Post-Surgical Recovery: Individuals looking to accelerate tissue repair and manage post-operative swelling through improved metabolic throughput.
- Neurological Recovery: Those managing the progression of Parkinson’s disease or recovering from a stroke can benefit from the neuroprotective and energy-boosting effects of transcranial PBM.
- Athletic Performance: Athletes utilizing light to reduce recovery time between high-intensity training sessions and manage exercise-induced muscle damage.
The Bottom Line: Precision Over Hype
Photobiomodulation is a legitimate, evidence-based frontier in neurorehabilitation, but it requires a departure from the "wellness" narrative. It is a biological tool that demands clinical precision, correct dosing, and a deep understanding of mitochondrial optics. While we are literally being starved of these wavelengths in our modern indoor lives, the key to reclaiming their benefits lies in professional application.
The science is clear: light can influence the very machinery of life. When applied within a comprehensive physical therapy framework, it serves as a powerful catalyst for recovery and long-term health.
Reframe Your Movement
If you are seeking a recovery strategy that bridges the gap between sophisticated laboratory science and practical clinical excellence, photobiomodulation may be the missing link in your rehabilitation. We invite you to book a clinical assessment at Unity Move Physical Therapy & Wellness to explore how we can integrate this technology into your personalized recovery plan.